AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
Back to Blog
Thyroid sick syndrome12/15/2023 
Finally, there is impaired transport of T 4 into peripheral tissues, such as the liver and kidney where much of the circulating T 3 is produced, further contributing to the decrease in production of T 3. Recent studies on postmortem tissues have confirmed that alterations in deiodinase enzymes occur in patients who died during an acute critical illness, with decrease in type 1 and increase in type 3 deiodinases and, surprisingly, an increase in skeletal muscle type 2 deiodinase. Additionally, since rT 3 is subsequently deiodinated by D1, degradation of rT 3 decreases and levels of this inactive hormone rise in proportion to the fall in T 3 levels. In contrast, inner ring deiodination by D3 may be increased by acute illness, resulting in increased levels of rT 3. D1 is inhibited by a wide variety of factors, including acute illness ( Table 107.1), resulting in the acute decrease in T 3 production in critically ill patients. One of the initial alterations in thyroid hormone metabolism in acute illness is the acute inhibition of type 1 deiodinase, resulting in the impairment of T 4 to T 3 conversion in peripheral tissues. Under normal conditions, ∼ 41% of T 4 is converted to T 3, ∼ 38% is converted to rT 3, and ∼ 21% is metabolized via other pathways, such as conjugation in the liver and excretion in the bile. The actions of D3 also include the inactivation of T 3 to form T 2, another inactive metabolite. Type 3 deiodinase is expressed primarily in the brain, in skin, and in placental and chorionic membranes. It is upregulated in hyperthyroidism and downregulated in hypothyroidism. Type 1 deiodinase (D1) is found most abundantly in the liver, kidneys, and thyroid. Removal of the inner ring, or 5-, iodine by type 3 iodothyronine deiodinase (type 3 deiodinase, D3) is the “inactivating” pathway, producing the metabolically inactive hormone, 3,3′,5′-triiodothyronine (reverse T 3, rT 3). Removal of the 5′-, or outer ring, iodine by type 1 iodothyronine 5′deiodinase (type 1 deiodinase, D1) is the “activating” metabolic pathway, leading to the formation of T 3. At least three deiodinases, each with its unique expression in different organs, catalyze the deiodination reactions involved in the metabolism of T 4. 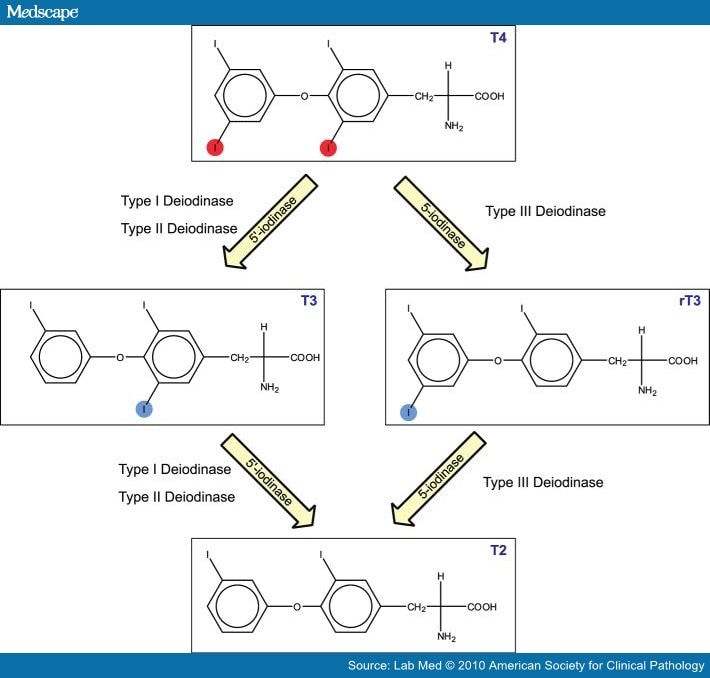
The major pathway of metabolism of T 4 is by sequential monodeiodination ( Fig. Thus, the sick euthyroid syndrome should not be viewed as an isolated pathologic event but as part of a coordinated systemic reaction to illness that involves both the immune and endocrine systems. Similar changes in endocrine function have been shown experimentally by the administration of cytokines from the interleukin (IL) and interferon families as well as tumor necrosis factor-α (TNF-α). These changes are rarely isolated and often are associated with alterations in other endocrine systems, such as reductions in serum gonadotropin and sex hormone concentrations and increases in serum corticotropin and cortisol levels. Because a wide variety of illnesses tend to result in the same changes in serum thyroid hormones, such alterations in thyroid hormone indexes have been termed the sick euthyroid syndrome or, more recently, the nonthyroidal illness syndrome. Despite abnormalities in serum thyroid hormone parameters, there is little evidence that these patients have clinically significant thyroid dysfunction. These effects are nonspecific and relate to the severity of the illness. 
There's more to see - the rest of this topic is available only to subscribers.Critical illness causes multiple alterations in thyroid hormone concentrations in patients who have no previously diagnosed intrinsic thyroid disease. Unless there is historic or unequivocal clinical evidence of hypothyroidism, thyroid hormone should not be administered and thyroid function tests should be repeated after recovery. The pathogenesis of this condition is not fully understood but may involve altered binding of T 4 to TBG and effects of high glucocorticoid and cytokine levels. TSH levels may range from 20 mU/L, with normalization after recovery from illness. More ill pts may additionally have a fall in total T 4 levels, with normal free T 4 levels. 
This is considered an adaptive response to a catabolic state. The most common pattern in sick euthyroid syndrome is a decrease in total and free T 3 levels, with normal levels of TSH and T 4. Therefore, the routine testing of thyroid function should be avoided in acutely ill pts unless a thyroid disorder is strongly suspected. Any acute, severe illness can cause abnormalities of circulating thyroid hormone levels or TSH, even in the absence of underlying thyroid disease.
0 Comments
Read More
Leave a Reply. |
 RSS Feed
RSS Feed
